Cramping, shots and hope: What it was like to freeze my eggs at age 35 during a global pandemic
Kaylee Hartung is an ABC News correspondent based in Los Angeles. At the age of 35, Hartung decided to undergo the process of mature oocyte cryopreservation, or egg freezing. She did so during the global coronavirus pandemic, which she also covered on the front lines for ABC News.
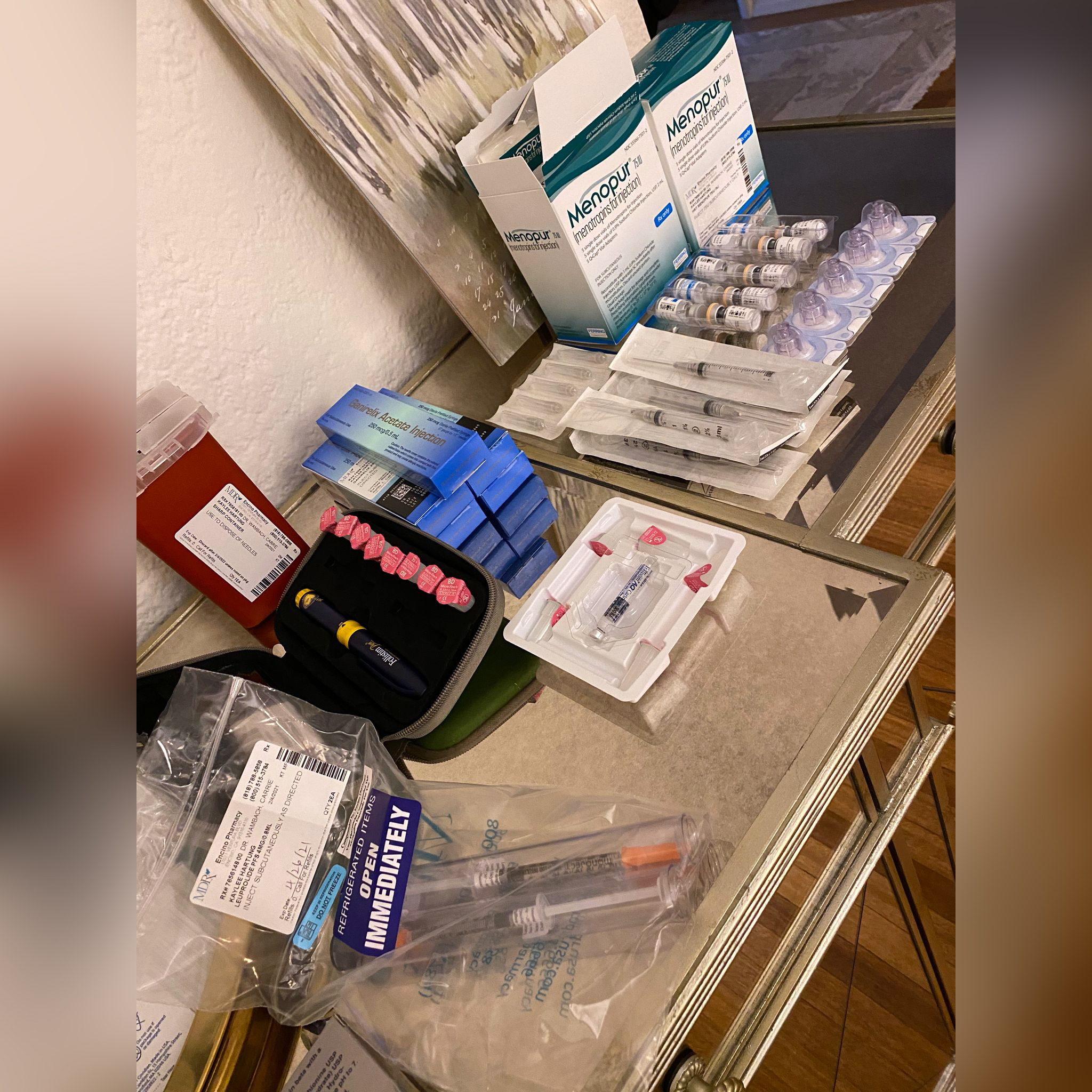
Hartung shared a photo on Instagram of the 27th and final injection she gave herself leading up to the egg retrieval procedure. Here, she shares more of her story.
After a 15-hour work day, highlighted by an interview with the governor of California for World News Tonight, I crawled into bed tired and sore, clutching my stomach.
The next morning I stumbled out of bed, still exhausted, and headed straight to the refrigerator to grab the 27th shot I would give myself in 12 days.
This was the last step in the month-long process of preparing my body for the now-standard practice of egg retrieval and freezing.
After the final injection into my abdomen, I was both relieved and proud of myself, but also anxious and overwhelmed. Recognizing it was a moment full of feelings I needed to remember, I took a photo.
It’s now been four weeks since my eggs were harvested and put into storage.
That concept feels strange, even surreal, but also brings me tremendous comfort knowing I have taken a piece of my future into my own hands. Every woman’s fertility journey is unique, and it’s oftentimes difficult to talk about.
When I first shared that photo and my experience on Instagram, I hoped it would encourage other women who are exploring this option. I did not anticipate the magnitude of the response that followed: The outpouring of support I received, the number of friends who also made this choice and the stories that strangers -- men and women -- felt compelled to share after reading mine.
Finding out I was the 'right' candidate for egg freezing
My mom was 25 when she gave birth to me. Growing up, I imagined I would follow a similar timeline.
My 20s came and went, and I’ve spent the past decade unapologetically prioritizing my career over my personal life
But my 20s came and went, and I’ve spent the past decade unapologetically prioritizing my career over my personal life. I am happy and satisfied in so many ways, but as cliched as it sounds, there’s no denying the cruelties of the biological clock.
So during a regular checkup a couple of years ago, I casually asked my gynecologist about the idea of freezing my eggs. I was disarmed when she replied something to the effect of: “I’m so glad you asked. This is the perfect time to do it.”
I’m not sure who I thought was the “right” candidate to freeze their eggs, but it came as a shock that it was me, then 33, who fit the bill.
And yet, for the next two years I came up with a litany of excuses not to do it. The shots, a surgery and recovery would interrupt my unpredictable and demanding work schedule. Where would I find the time? I had fears about how the flood of hormones might affect my body, the weight I thought I would gain and the emotional whirlwind I was afraid of getting caught in.

Then there was the cost. The five-figure price tag, coupled with the frustrating discovery that my otherwise very good health insurance plan wouldn’t cover any of it, became the largest obstacle.
Even with advances in technology, scale and accessibility, egg freezing typically costs between $10,000 and $20,000 out of pocket, and that’s if you’re lucky enough to have enough eggs retrieved through one round of treatment. Plus, storing your eggs can cost up to $1,000 per year.
Taking out a loan and starting the process
As I turned 35 in a year where so much seemed to be out of our control, I decided to get serious with myself and make a plan: Logistically, financially and emotionally. Somewhere between rallying the support of my closest friends, taking out a substantial personal loan and leaning on the stability of a supportive workplace, I decided to go for it.
A video consultation with my fertility specialist kicked off the process and began my education.
For eight to 13 days I would be injecting myself with medication to stimulate my ovaries to mature multiple eggs at once, with the goal of harvesting eight to 10 eggs. But it won’t be until I’m ready to thaw and fertilize the eggs that we’ll know anything about the eggs’ quality.
My first question: "How soon do we know how many eggs I’ll have?” We got an indication a few days later during my initial office visit, with the help of an ultrasound to count my ovary follicles and blood tests to measure my hormone levels.
It’s astounding how little I knew about my own body before that moment
Leading up to that fertility test, the worst case scenarios ran through my head. What if my ovaries didn’t work? What if I didn’t have very many eggs or any at all? I know more women than I can count who’ve been challenged with infertility and faced heartbreak in the process. So I had a pang of guilt accompany the wave of relief I felt when I learned my reproductive system was healthy.
In hindsight, it’s astounding how little I knew about my own body before that moment.
Through nine days of estrogen pills to “sync” my follicles and prepare them for the egg growth, I developed an insatiable hunger and the bloating began. A subsequent ultrasound signaled that it was time to begin the next stage -- what I thought would be the hard part.
Although I like to think I thrive under pressure, let me tell you, finding myself alone at home, unpacking boxes of syringes, needles and medicine vials in my living room, I was more than intimidated. Over and over, I watched YouTube “how-to” videos for assembling the shots. Graciously one of my girlfriends stayed on the phone and talked me through my nerves.

Two days in, I was comfortable injecting the shots. The bloating was making my body quickly feel unfamiliar, but it was manageable. In between assignments for work, I squeezed doctor’s visits in every three days for more ultrasounds and blood tests to monitor the eggs’ growth. I wondered, what was I ever so afraid of?
Then one week in, some cosmic combination of pandemic solitude and all those extra hormones hit hard. I woke up on a Saturday with no desire to get out of bed, and spent the rest of the day on the couch, sobbing, as I binged old episodes of "Grey’s Anatomy."
After 12 days of shots, I was put under anesthesia at a surgical center. My doctor guided a needle into my ovaries to gently suction each egg from its follicle.
When I woke up 45 minutes later, I was told the procedure had been a success! A batch of my eggs was now safely sitting in a freezer somewhere, and I could get back to the life I knew before hormone injections. I knew the recovery would mean a few days of taking it easy, and I figured I could safely celebrate with my first glass of wine in a month that night. Not so fast, I was told.
I was informed that I was at risk for ovarian hyperstimulation syndrome, or OHSS. It’s a complication that can occur after fertility treatments, and my doctor said the best way for me to protect myself from it was to completely eliminate carbohydrates and sugars for the next 10 to 14 days. As unrelenting nausea set in, all I craved was a piece of toast, not the leafy greens and lean protein I was instructed to eat.
The intense cramping was unlike anything I had experienced in my life
Four days later I was still camped out on my couch, in a miserable mood with a heating pad across my torso. The intense cramping was unlike anything I had experienced in my life. I found it tough to attend to basic emails, and I silenced the phone calls of concerned family and friends. My closest friends in Los Angeles offered to visit, but all I wanted was to be alone.
What turned into a week-long recovery was by far the most taxing part of the entire six-week process.
As I write this, my body and mind are back on even ground. And the resounding feeling I have is that whatever discomfort I endured was worth it.

I don’t even know if I’ll ever use these eggs, but it’s empowering to know I’ve given myself a better chance of bringing healthy eggs to the table when the time is right. Still, there are no guarantees.
Deciding to share my experience
Egg freezing is often referred to as something of an “insurance policy” for getting pregnant on your own timeline, but according to the Mayo Clinic, the chances of becoming pregnant after a frozen egg is implanted are only 30 to 60%. These odds can be affected by multiple factors, including a woman's age and health.
"You have to be realistic," explains Dr. Jennifer Ashton, ABC News chief medical correspondent and a board-certified OBGYN. "This is not a guarantee of a live birth or the family of your dreams down the road. It is one important piece of it, and it’s great that now we’re starting to see a shift in paradigm from treating infertility to being proactive about fertility."
It turns out I’m just one of many women who’ve made this choice in the middle of a pandemic. Between June and December of 2020, the Langone Fertility Center at New York University saw a 32% increase in women freezing their eggs. More women are opting into this procedure -- despite the time, money and discomfort required -- than ever before.
And yet, the response I kept getting to my initial post was, "Thank you for talking about this.”
Thank you for talking about this
I hope that by sharing my own experience I can play a small part in normalizing the conversation around fertility. I also want to remind women who put their bodies and minds through this tremendous stress: You're not alone.
Visit GoodMorningAmerica.com/infertility for more resources and information on fertility treatments.
Editor's note: This story was originally published on March 17, 2021.




