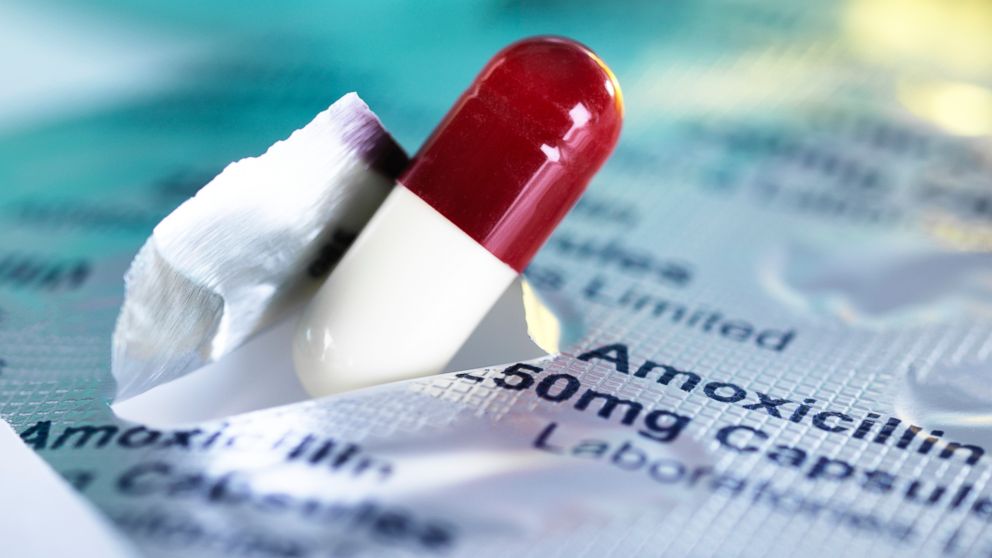
Antibiotics are overprescribed: Here's why that's not good, and what you need to know
Coughing, headaches, runny noses. Nobody likes to feel sick, so they turn to a doctor for advice.
With people more frequently turning to urgent cares and retail clinics to seek healthcare when they get sick, experts are starting to examine the effect of antibiotics prescribed in these settings.
New research from the Centers for Disease Control and Prevention (CDC) in Atlanta, Georgia, University of Utah, and The Pew Charitable Trusts suggests that doctors may be overprescribing antibiotics, both in urgent care and retail clinic settings and in more traditional medical spaces: emergency rooms and doctor’s offices.
A study published in the Journal of the American Medical Association – Internal Medicine reveals the statistics. Dr. Katherine Fleming-Dutra and her research team showed that for respiratory or airway tract related illnesses, antibiotic medications were inappropriately prescribed in 45.7 percent of urgent care visits, 24.6 percent of emergency room visits, 17 percent of medical office visits and 14.4 percent of retail clinic visits.
“There is a lot of room to improve outpatient antibiotic prescribing. All of these settings have room to improve,” Fleming-Dutra, the lead investigator of the study and the Deputy Director of the CDC Office of Antibiotic Stewardship, told ABC News.
Every doctor and patient wishes for a pill that could cure any pain or symptom, but researchers are continuing to find evidence that extra care needs to be taken with antibiotic prescriptions.
What are antibiotics?
They fight what are often called “germs:” bacteria. But people can become infected with viruses, fungi, or parasites as well, and antibiotics don’t work against those.
The CDC definition: A type of drug that can kill or stop the growth of bacteria. An example would be penicillin.
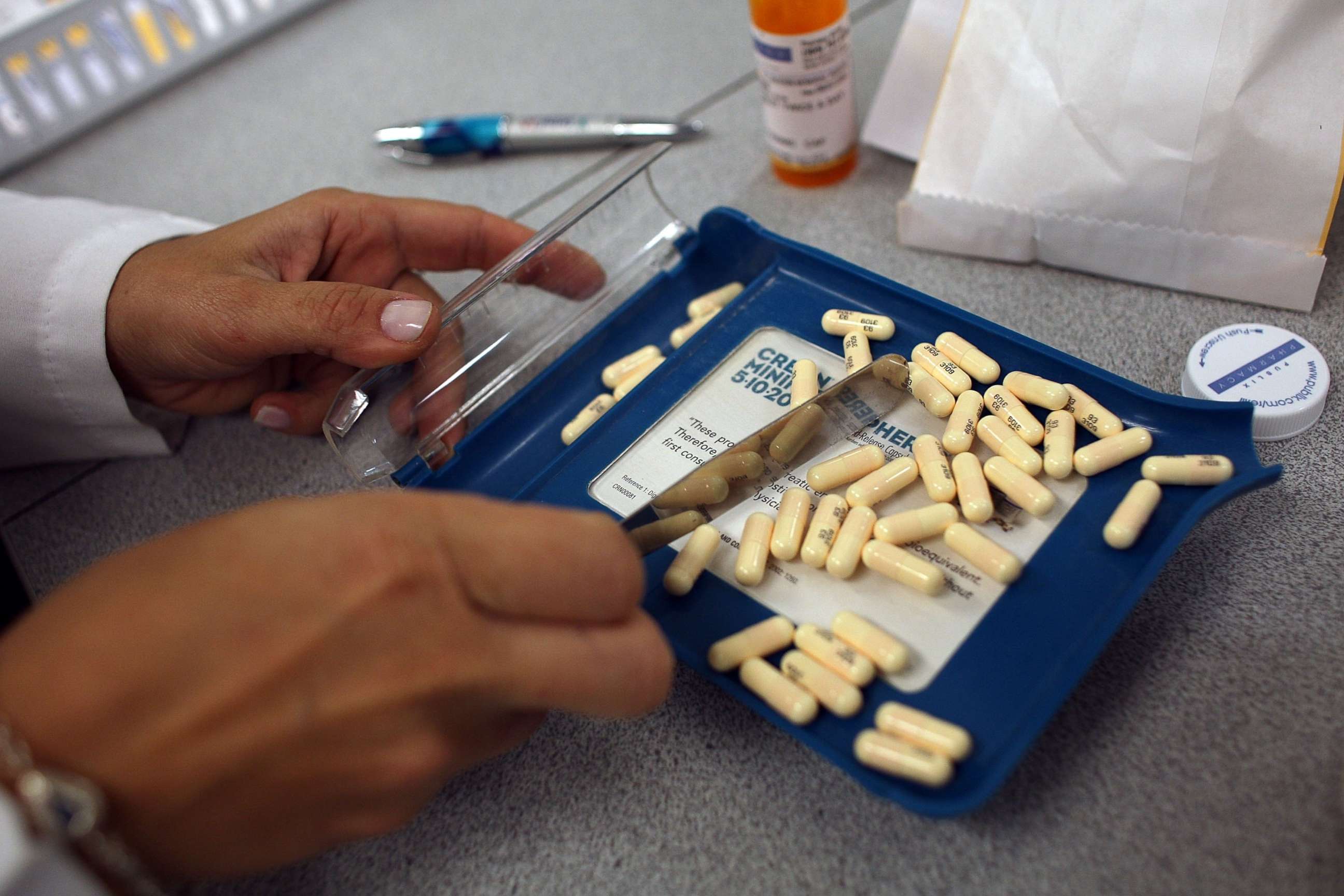
What is antibiotic resistance?
If a medication kills almost all of the bacteria present during an infection, sometimes a few might survive – they have adapted themselves to survive the antibiotic.
When this happens, that adapted, resistant germ can continue to multiply and the infection can grow. Eventually, the new bacteria may spread to other people or animals – and the original antibiotic doesn’t work against it.
Over 2 million people every year become infected with bacteria that are resistant to antibiotics, according to the CDC. Over 23,000 people die as a direct result of these infections every year.
What is a superbug?
A superbug is a bacteria that has high levels of resistance to many different antibiotics.
One example: drug resistant Neisseria gonorrhoeae, the bacteria that causes gonorrhea, a sexually transmitted infection. The CDC reports 246,000 cases of drug-resistant gonorrhea infections per year.
Why is unnecessary antibiotic use a problem?
“Antibiotics are life-saving medications,” Fleming-Dutra said. “They are very important to medicine and medical care. They allow us to prevent and treat bacterial infections. They allow us to treat people with cancer, chemotherapy, and surgery who depend on the ability to prevent and treat infections. That is why resistance is such an important issue.”
Unnecessary antibiotic use directly contributes to antibiotic resistance. When people take antibiotics more frequently, it provides more chances for bacteria to adapt and learn to fight off modern drugs. There are currently a limited number of different antibiotics and scientists are having a hard time creating new drugs that can keep up with new superbugs.
Unnecessary antibiotics can harm people as well. “All antibiotics, like all medications, have side-effects and risks,” said Fleming-Dutra. They can cause “mild side-effects like rashes or yeast infections” or “quite serious reactions that are life-threatening.”
Antibiotics can kill helpful bacteria and make it more likely for us to develop a harmful bacterial infection. Clostridium difficile or “C. difficile” is directly related to antibiotic use and contributes to 250,000 illness and 14,000 deaths per year, according to the CDC. C. difficile is the scourge of hospitals and results in over $1 billion in preventable medical costs per year.
When do people not need antibiotics?
Since antibiotics only work against bacterial infections, common illnesses that are caused by viruses do not benefit from antibiotic use.
That includes the common cold, most cases of sore throat (known as viral pharyngitis), and chest colds (known as acute bronchitis). They are not caused by bacteria. Antibiotics will not be helpful for any of these conditions.
How big a problem is overprescribing?
People want an answer when they are sick; if they go to the doctor, they want to come out with a prescription. But prior research from the CDC suggests that 30 percent of antibiotic prescriptions in doctor’s offices, hospital-based clinics, and emergency departments are not needed.
Then why do doctors do it?
Doctors are trained to know when antibiotic medications are necessary. However, they often prescribe medications because they have preconceived thoughts about what patients want and strive to provide satisfying customer service.
“We know from previous research doctors are more likely to prescribe an antibiotic if they think a patient might want one,” Fleming-Dutra said.
What can be done about it?
A multi-pronged approach is necessary, according to the CDC.
The CDC encourages appropriate antibiotic use: starting drugs only when necessary and stopping at the right time. They are working with organizations such as the Urgent Care Association of America to promote the appropriate use of antibiotics.
What you need to know and what you can do?
The best thing a patient can do is talk to your doctor. “Ask when antibiotics are needed and not needed,” suggests Fleming-Dutra. “Do not pressure your healthcare provider to prescribe medications but ask 'What can I do to feel better?' Ask when you should return if you do not get better or if your symptoms get worse. Communication is key."
It is also important to take medication as prescribed. Take it exactly as directed, the entire course of medications, so there is none left over to “save.” Never take someone else’s medications and do not share antibiotics.
Of course, an ounce of prevention is better than a pound of cure. Fleming-Dutra recommends steps to limit spreading germs in the first place. “Washing your hands, covering your cough and staying home when you are sick. And of course getting recommended vaccines.”
Michael MacIntyre, M.D., is a psychiatry resident working in the ABC News Medical Unit.