I lost my pregnant wife to COVID-19. This is what I want people to know.
Juan Duran-Gutierrez is now a single father raising three young children, including a newborn, after his wife, Aurora Chacon-Esparza, died of COVID-19 during the global coronavirus pandemic.
Chacon-Esparza was healthy and following safety precautions, according to Duran-Gutierrez, when she contracted COVID-19 in June while seven months pregnant with the couple's third child together.
"I really thought she was going to pull through," Duran-Gutierrez, of Minnesota, told "Good Morning America." "She’s always been a really strong woman. She didn’t have any pre-existing conditions. She was healthy."
Chacon-Esparza, who would have turned 36 in August, was hospitalized on June 14 after one week of isolating with COVID-19 symptoms at home, along with other family members who had also been exposed to the virus, according to Duran-Gutierrez.
Just around five days later, Chacon-Esparza was placed on a ventilator.
"She continued to get short of breath and her lung disease worsened to the point where she was struggling to breathe," said Dr. Todd Stanhope, the OBGYN who treated Chacon-Esparza at North Memorial Health in Brooklyn Center, Minnesota. "I counseled both her and Juan the day that she was intubated that she was struggling to breathe and without intubation, she would have exhausted herself trying to breathe."
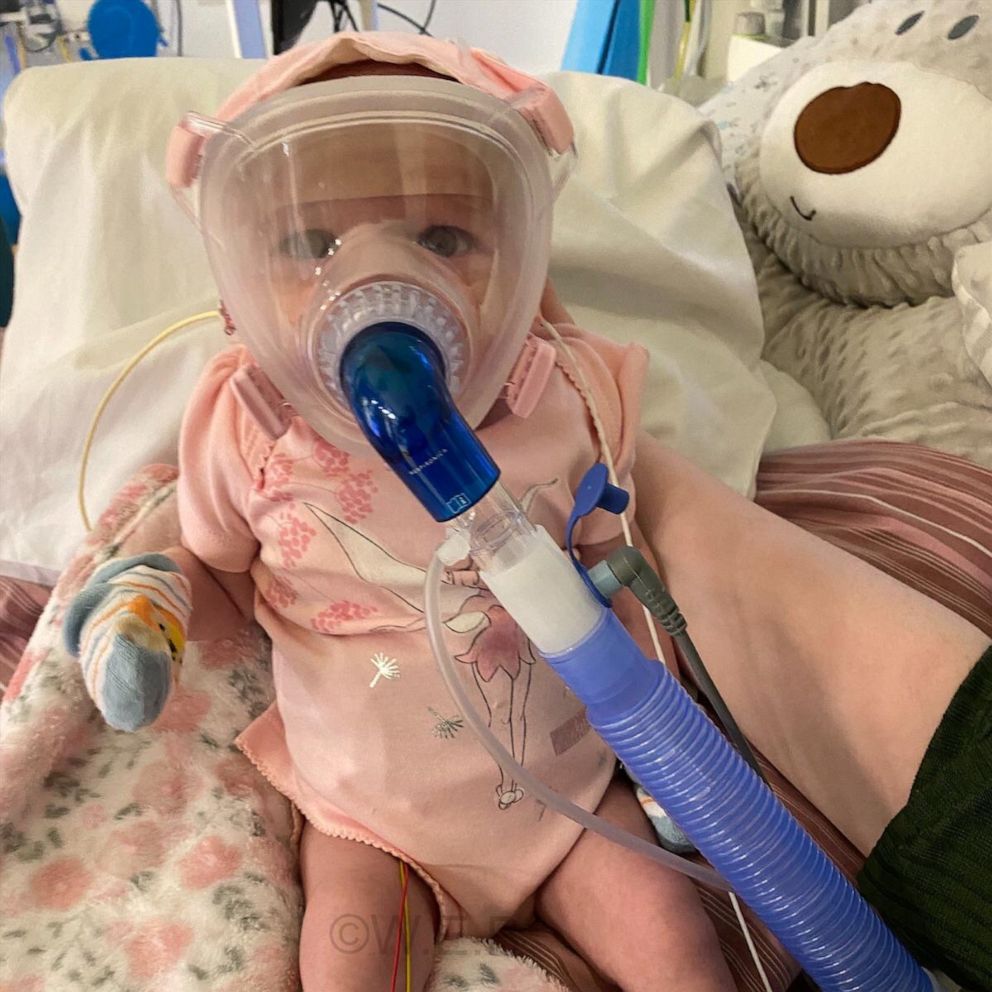
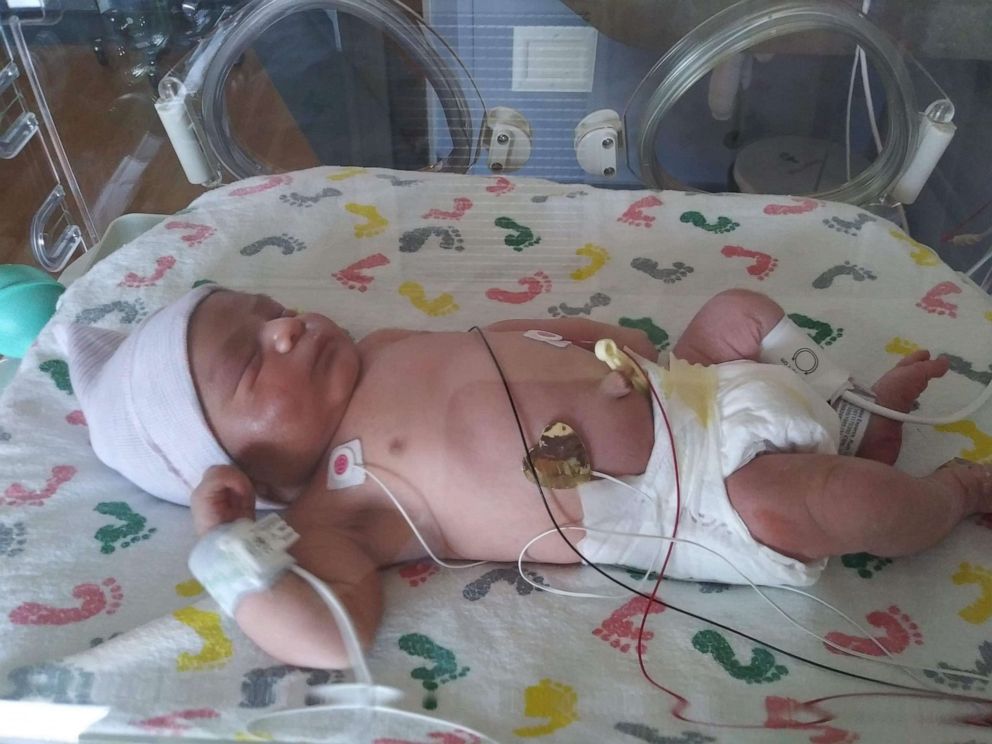
Shortly after being intubated, Chacon-Esparza had to undergo an emergency cesarean section to deliver her third child, a healthy baby girl that Duran-Guiterrez named Andrea.
The baby, who tested negative for COVID-19, was born at 30 weeks weighing 4 pounds, according to Stanhope, who performed the emergency C-section.
Less than one month after giving birth, Chacon-Esparza passed away, leaving behind a husband, three children ages 7 and younger, two older stepchildren and her extended family.

"I thought until the end that she was going to make it," Duran-Gutierrez said of his wife, whom he was able to finally see in the hospital just before she passed away. "I was holding her hand and talking to her."
"She really took care of herself," he said. "She protected herself whenever she went out, I’m talking face masks, and she had a whole bunch of hand sanitizers and hand wipes in her SUV, so she was really taking care of herself."
The impact of COVID-19 on pregnant women
Just as Duran-Gutierrez, a Lyft driver, is now looking ahead to his future as a single dad, he is also coming to terms with what he now knows about how COVID-19 affects pregnant women.
"For pregnant women, be very careful," he said. "I’m not trying to alarm anybody when I share this story. I don’t want pregnant women to feel like it’s going to happen to them, but they should take all the precautions because it could happen to them."

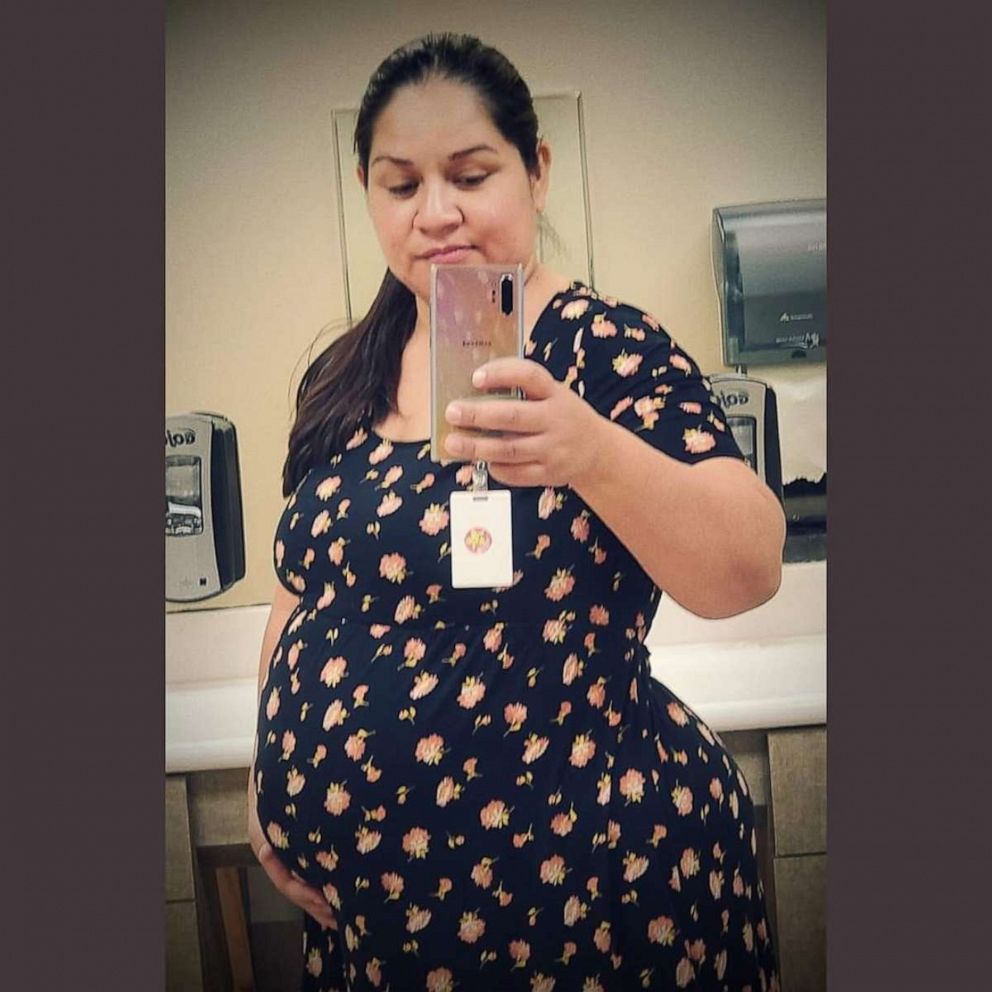
For 35-year-old Ruth González Esparza, her bout with COVID-19 came in the 38th week of her pregnancy.
The mother of two told “GMA” through a translator that she never thought she would be infected by the virus, though she was admitted to Denver Health in Colorado, after having a sore throat. She tested positive for COVID-19 immediately following the birth of her son, Jose Luis Sanchez González, on March 31.
Esparza had a normal labor and delivery with no symptoms, according to Denver Health. It was only after her delivery that Esparza began feeling symptoms that included fever, cough and muscle pain.
"I also had high blood pressure and the baby’s heart rate was very low," Esparza said, adding that she was afraid, even for her 5-year-old daughter who was at home.
"We didn’t know this could happen to us," she said. "You immediately think the worst and all the news scared me even more."
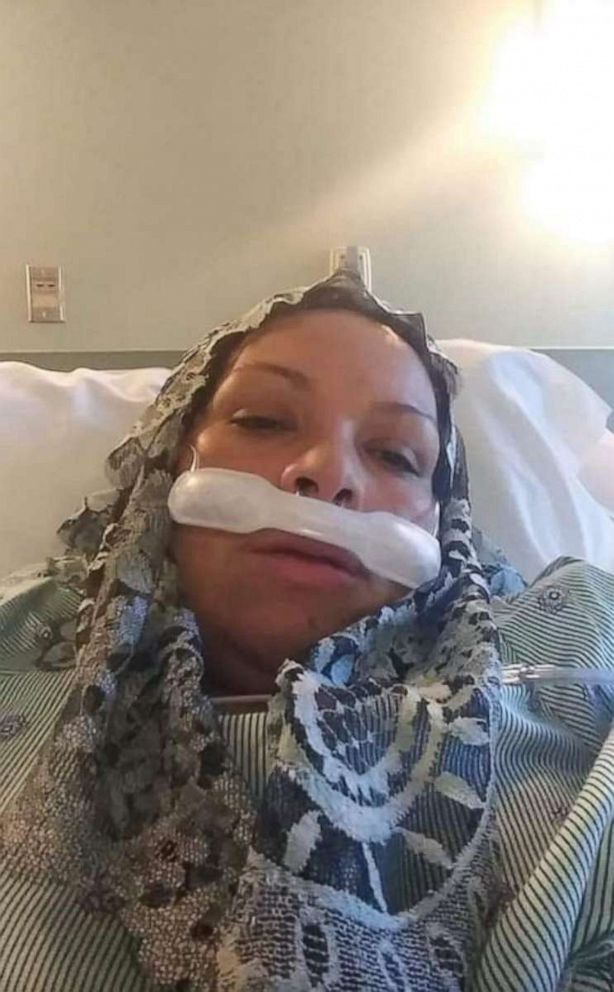
Esparza was one of the first mothers to have COVID-19 at Denver Health. After she tested positive, she was intubated in the intensive care unit for two weeks and separated from her newborn for one month.
Esparza made the decision to separate from him for protection.
"I felt mentally very sad, depressed, scared because even though I had a lot of faith in God, I was scared; every day I didn’t get better is another day that I felt more sick, more tired and the only thing that keep me going was the calls with my mom, with my husband and with my daughter, Kerem," Esparza said.
More than 26,000 pregnant women in the United States have been diagnosed with COVID-19 since January and 45 pregnant women have died due to complications from the virus, according to the U.S. Centers for Disease Control and Prevention (CDC).
Among the diagnosed cases of pregnant women with COVID-19, an overwhelming majority were, like Esparza and Chacon-Esparza, women of Hispanic and Latina descent, according to the CDC.
In a study released this summer, researchers at the University of Pennsylvania found the rate of virus exposure among Black and Hispanic women to be five times higher than among white and Asian women.
Researchers have not yet determined why Hispanic women are disproportionately affected by COVID-19, according to Dr. Rashmi Rao, a maternal-fetal medicine specialist at UCLA Medical Center in Los Angeles.
"There could be an increased amount of pre-existing conditions. It could just be that there are racial disparities in care in the United States," Rao told "GMA." "Some of it has to do with social determinants, like socioeconomic status or possibly the way people are cohorted in certain areas in the country, where depending on how many people live with you, can you really socially distance, and that may be present in some populations more than others."
"There are many theories, but the truth is from a science standpoint, we have not concluded anything based off a certain race that would make them more predisposed to it just based on their racial background or ethnicity," she said.
More than eight months into the virus hitting the U.S., there are also still many questions remaining for all pregnant women about how they could be impacted by COVID-19.
"What I’ve been telling my patients is the one thing I can tell you for sure is that pregnant women get COVID," said Rao. "Everything else I think is still a little bit of conjecture."
Researchers are learning as they go when it comes to how COVID-19 affects pregnant women because the virus is still relatively new and full-scale studies are just underway.
For instance, roughly nine months into the pandemic, researchers are just now able to see what complications, if any, there are at delivery for women who contracted COVID-19 early on in their pregnancy, according to Rao.
"That's another concern that pregnant women have and I’ve had to tell them that we’ll have to wait on this," she said. "As of right now, there’s nothing overwhelmingly glaring to us about the baby’s birth weight or birth timing but stay tuned because we are keeping a close eye on that."
What doctors do know is that pregnancy causes changes to the immune and respiratory systems, which has led to speculation that pregnant women might be more vulnerable to the disease.
Dr. Amesh Adalja, a senior scholar at the Johns Hopkins University Center for Health Security, agreed. Adalja's work focuses on infectious disease and pandemic preparedness.
"We tend to be more cautious of pregnant women because pregnant women are considered immunosuppressed and they also have physiological changes, as they go along in their pregnancy," Adalja told "GMA," adding that there's still a lack of data. "It makes them more prone to get into respiratory distress quicker."
Adalja said pregnant women with COVID-19 may be mere likely to be admitted to the ICU, since doctors are watching these patients closely considering we're dealing with a novel disease.
"We're cautious with pregnant women but what we've seen so far, is not necessarily the same with what we've seen with for example, Zika or the same with influenza," Adalja said.
One recent study on non-hospitalized pregnant women found that symptoms for pregnant women with COVID-19 can be prolonged, lasting two months or longer for a quarter of the women who participated in the study.
The common early symptoms for pregnant women were cough, sore throat, body aches and fever, according to the study, all symptoms felt by Chacon-Esparza before she was hospitalized.
"It all started with body aches, then the nauseous came, a lot of coughing, high fevers and then shortness of breath, which is the reason she went to the hospital," Duran-Guiterrez said of his late wife. "She was admitted immediately because her oxygen was pretty low."

A study in June from the CDC found that while pregnant women don't seem any more likely to die of COVID-19 than other groups, they do appear to be more likely to become extremely sick, and even become hospitalized, once they get infected.
Despite worse symptoms seen in pregnant women with COVID-19, there was no difference in the risk of death between pregnant and non-pregnant women with COVID-19, the study found.
While every woman needs to consult with her own doctor, there so far is no broad evidence to suggest that otherwise healthy women should avoid getting pregnant during the pandemic, according to Rao, who emphasizes that getting pregnant is a very personal decision for each woman and her doctor.
"From a health standpoint, we are not recommending that people delay pregnancy for COVID, mostly because this isn’t getting better anytime soon and as of right now we are not seeing any overwhelming reason why pregnancy in and of itself is causing an increased risk or susceptibility to COVID," said Rao. "If that data were to come out, sure we might make different recommendations, but right now, from a health standpoint, there’s no contraindications to getting pregnant at this time."
After a month-long stay in the hospital, Esparza was released as doctors continued to monitor her recovery process. She is now doing well and raising her children with her husband, Federico González.

Esparza's message to expectant mothers is to wear a mask and visit your doctor if you feel any symptoms of illness.
"Especially if you have complications, take care of yourself," she said. "You owe it to your baby to not become one of the statistics."

5 tips for moms-to-be
If a woman is pregnant during the pandemic, there are things she should do to help keep herself safe throughout her pregnancy.
Here are five tips from experts.
1. Wear a face mask and practice good hand hygiene: "Face coverings are a must and frequent hand washing is an absolute must and that’s probably one of the most important things," said Rao.
For hand washing, CDC guidelines are to wash hands with soap and water for at least 20 seconds, or use hand sanitizer with at least 60% alcohol if soap and water are not available.
Face masks should be worn in addition to "prevention actions like washing hands frequently and avoiding close contact with other people," according to the CDC. Pregnant women should both wear masks themselves and avoid contact with others who are not wearing masks.
2. Practice social distancing: Pregnant women should limit their travel and try their best to avoid outings in places where they cannot social distance, according to Rao.
The CDC recommends that pregnant women say at least 6 feet away from people outside their household.
3: Continue with all doctors' appointments: Pregnant women should not skip routine healthcare appointments or avoid going to the hospital in an emergency, experts say.
If you have concerns because of COVID-19, the CDC recommends that women talk with their health care providers ahead of time about what protocols they have in place to keep healthy patients away from those who may be sick and to minimize any potential exposure to COVID-19.
4. Quarantine before delivery: "For the mom or parents or anyone who is going to be in contact with the child, it’s important to quarantine around the delivery time so that way the baby is not exposed after birth," said Stanhope.
5. Get recommended vaccines: The CDC recommends that women get vaccinated against influenza during pregnancy, as well as the whooping cough (Tdap) vaccine.
What to know about coronavirus:
- How it started and how to protect yourself: coronavirus explained
- What to do if you have symptoms: coronavirus symptoms
- Tracking the spread in the US and Worldwide: coronavirus map